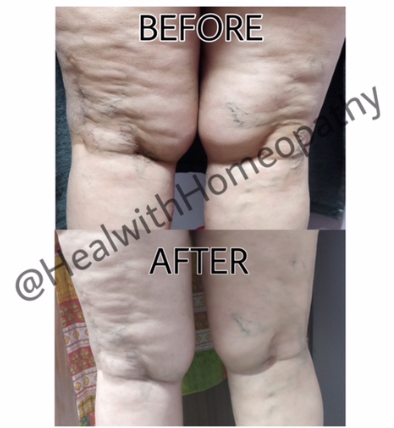
 A vein is called ‘varicose’ when it is dilated and tortuous. There are various places in the body where veins show tendency towards varicosity e.g. veins of the lower limb, spermatic veins, esophageal veins and haemorrhoidal veins.1
A vein is called ‘varicose’ when it is dilated and tortuous. There are various places in the body where veins show tendency towards varicosity e.g. veins of the lower limb, spermatic veins, esophageal veins and haemorrhoidal veins.1
AETIOLOGY
Varicose veins mostly occur due to incompetence of their valves. It occurs commonly in those whose works demand standing for long hours e.g. conductors, drivers of the trams etc. Yet it is not uncommon in women. These are tone and contractility of the muscles of the lower limb being encircled by a tough deep fascia. Incompetence of valves, which may be a sequel of venous thrombosis, seems to be the most important factor in initiating this condition. Varicosity may also be secondary, predisposed by any obstruction which hampers venous return e.g. tumors. A hormonal factor gives an indication of occurrence of this disease in females. In younger age group congenital arteriovenous fistula may be the cause of varicose vein.1
HISTORY
- Age -Though varicose vein can affect individuals of all age groups, yet middle-aged individuals are the usual sufferers.1
- Sex – Women are affected much more commonly in the ratio of 10: 1.1
- Occupation – Certain jobs demand prolonged standing e.g. tram drivers, policemen, conductors, etc. and the persons involved in these jobs often suffer from varicose veins. Varicose veins may also occur in individuals involved in excessive muscular contractions e.g. Rickshaw-pullers and athletes. It is doubtful if these occupations cause the varicose veins or they just exacerbate the symptoms already present.1
SYMPTOMS
- The commonest symptom is the pain which is aching sensation felt in the whole of the leg or in the lower part of the leg according to the position of the varicose vein particularly towards the end of the day. The pain gets worse when the patient stands up for a long time and is relieved when he lies down.1
- Asymptomatic varicose veins are also seen in cases where there are painless varicose veins on one side and severe symptoms with very few visible varicose veins on the other side.1
- Patient may complain of bursting pain while walking, which indicates deep vein thrombosis. Night cramps may also be present. The ankle may swell towards the end of the day and the skin of the leg may be itching. Some patients complain of severe cramps at nights. Varicose ulcer may be seen on the medial malleolus.1
A few questions should be asked1
(i) Any difficulty in standing or walking, which indicates presence of deep vein thrombosis.
(ii) Any additional complaint should be enquired other complaint than varicose vein itself. For example, if the patient is suffering from constipation or a swelling in the abdomen, it may be a cause of secondary varicose vein.
Risk factors
- Obstetric history of varicosities: Whether the patient suffered from ‘white leg’ during the previous pregnancies.
- Use of contraceptive pills for quite a long time, as this may cause deep vein thrombosis.1
PHYSICAL EXAMINATION
- Inspection
To be checked which vein has been varicosed–long saphenous or short saphenous or both. In case of the former a large venous trunk is seen on the medial side of the leg starting from in front of the medial malleolus to the medial side of the knee and along the medial side of the thigh upwards to the saphenous opening. This venous trunk receives tributaries in its course. In case of short saphenous vein varicosity the dilated venous trunk is seen in the leg from behind the lateral malleolus upwards in the posterior aspect of the leg and ends in the popliteal fossa.1
- Palpation- Examination of the varices is very important. The aim is to locate the incompetent valves communicating the superficial and deep veins.1
- Brodie-Trendelenburg test
- Tourniquet test
- Perthes’ test
- Perthes’ test (Modified)
- Schwartz test
- Pratt’s test
- Morrissey’s Cough Impulse test
- Fegan’s method to indicate the sites of perforators
- Percussion – If the most prominent parts of the varicose veins are tapped, an impulse can be felt by the finger at the saphenous opening. This is known as Schwartz test. Sometimes the percussion wave can be transmitted from above downwards and this will imply absent or incompetent valves between the tapping finger and the palpating finger.1
- Auscultation – The importance of auscultation is limited to the arteriovenous fistula, where a continuous machinery murmur may be heard.1
- Regional lymph nodes (inguinal) – are only enlarged if there be venous ulcer and thesis infected.1
- Other limb– should be examined for presence of varicose veins and different tests to exclude deep vein thrombosis, incompetent perforators and venous ulcer to plan treatment.1
COMPLICATIONS1
- Hemorrhage– it may occur from minor trauma to the dilated vein. The bleeding may be profuse due to high pressure within the incompetent vein. Simple elevation of the leg does a lot to stop such bleeding.1
- Phlebitis-This may occur spontaneously or secondary to minor trauma. Mild phlebitis may be produced by the sclerosing fluid used in the injection treatment. In this condition varicose vein becomes extremely tender and firm. The overlying skin becomes red and oedematous. Pyrexia and malaise may be associated with.1
- Ulceration– This is more due to deep venous thrombosis rather than varicose veins alone. The patients often give previous history of venous thrombosis suggested by painful swelling of the leg. After thrombosis has been reanalyzed the valves of the deep veins are irreparably damaged. The deoxygenated blood gets stagnated in the lower part of the leg particularly on the medial side where there are plenty of perforating veins. The superficial tissue loses its vitality to certain extent and a gravitational ulcer follows either spontaneously or following minor trauma. The majority of patients with venous ulcers have incompetent communicating veins. The arteries and nerves should be examined to exclude other causes ofulceration.1
- Pigmentation
- Eczema
- Lipodermatosclerosis – This means the skin becomes thickened, fibrosed and pigmented. This is due to high venous pressure which causes fibrin accumulation around the capillary and it also activates white cells.1
- Calcification of vein
- Periostitis in case of long-standing ulcer over the tibia
- Equinus deformity
CAUSES
Primary
The valves are incompetent both of the main vein and of the communicating veins. Venous walls may be weak which permit dilatation causing incompetence of valves. Very rarely there may be congenital absence of valves.1
Secondary1
1. Obstruction to venous outflow
- Pregnancy
- Fibroid
- Ovarian cyst
- Pelvic cancer (of cervix, uterus, ovary or rectum)
- Abdominal lymphadenopathy
- Ascites
- Iliac vein thrombosis
- Retroperitoneal fibrosis
2.Destruction of valve– from deep vein thrombosis.
3. High pressure flow – from arteriovenous fistula.
GENERAL TREATMENT
The chief general indication is to give the veins support, both in their tissues and externally. External; support is best afforded by an ordinary roller bandage, an elastic stocking, or an India-rubber bandage applied to the limb. The last is the best, as it is not only a support, but is actually curative in many instances. Rest in the recumbent positions is always a great help, and standing is of course bad. Where there is a tendency to varicose veins, much standing will be sufficient to cause them. But sometimes, in spite of most adverse conditions, medicines will affect a cure.3
SCOPE OF HOMEOPATHY
Varicose veins generally considered an irreversible condition can be benefitted from homeopathic remedies. Literature evidences use of homeopathy for varicose veins and also seen to be beneficial in reducing varicose ulcers, varicosities after oral and local application of homeopathic remedies. Medicine shall only be taken under supervision of a registered and skilled homeopathic practitioner. It shall be accompanied by auxillary measures of weight loss, bandage, resting in recumbent position and standing etc.
HOMEOPATHIC MEDICINES FOR VARICOSE VEINS
 Aesculus Hippocastanum 5
Aesculus Hippocastanum 5
Aching and soreness in limbs, in left acromion process with shooting down arms; finger tips numb.
 Calcarea Fluorica 2
Calcarea Fluorica 2
Varicose veins and their ulceration; vascular tumors with dilated blood vessels.
 Carbo Vegetabilis 2
Carbo Vegetabilis 2
Venosity with offensive, excoriating discharge, excoriations superficial and irregular in outline; inflammations sluggish, tending to suppuration or gangrene, with burning pain, great weakness and collapse; gastric disturbances with accumulation and passage of offensive flatus; varicose veins of genitals, with blueness and burning, bluish tumors (Carb. an., if they be indurated); ulcers, fistulae.
 Crotalus Horridus
Crotalus Horridus
Varicose veins, useful when indicated on generalities of patient.
 Ferrum Phosphoricum 2
Ferrum Phosphoricum 2
Varices and haemorrhoids in young people, costiveness, stool hard and difficult, followed by backache, throbbing pains.
 Fluoricum Acidum 2
Fluoricum Acidum 2
Varicose veins; little blue collections of veins in small spots; on legs to ulceration; flat naevus. Painful varicose veins. Wants to put feet out of bed at night.
 Pulsatilla Nigricans 2
Pulsatilla Nigricans 2
Disturbance of venous circulation; varicose veins in legs and about testicle of bluish hue, with soreness and stinging pains; passive haemorrhages.
 BENEFICIAL FOODS
BENEFICIAL FOODS
Constipation is thought to increase pressure on the veins in the legs, leading to the formation of varicose veins. A fiber-rich diet decreases constipation and helps to prevent varicose veins.4
- Wholegrain breakfast cereals, whole meal bread sand rolls, brown pasta, and rice are recommended to help bulk the stools and prevent constipation. Cereals rich in insoluble fiber bulk the stools and bind water. The resulting larger, softer stool is much easier to pass, leading to less straining and Iess pressure on the leg veins. On increasing fiber intake in the diet, water intake should also increase, to at least six cups or glasses a day.4
- Green leafy vegetables and cruciferous vegetables such as broccoli and Brussels sprouts help to bulk the stools with the insoluble fiber that they supply.4
- Citrus fruits such as oranges and grapefruits, and raspberries, blackcurrants, strawberries, peppers, and green leafy vegetables all supply vitamin C. This vitamin is vital for maintaining the strength of collagen, the material that helps to support vein walls. A lack of vitamin C in the diet leads to the breakdown of small veins, which may worsen varicose veins.4
- Bilberry extract contains antioxidants called anthocyanidins, which have been shown to decrease the leakage of tiny blood vessels in people with varicose veins. The anthocyanidins seem to be able to help mend the damaged connective tissues in the capillary walls of the veins that make the veins bulge and protrude. Eating bilberries may have similar effects.4
- Nuts, seeds, and oily fish contain essential fatty acids and eating some of these foods each day helps to strengthen the capillary walls of veins.4
- Beets–Contain betacyanin, phytochemical compound that can drastically lower the levels of homocysteine in the body. Homocysteine is a natural amino acid can harm blood vessels.
- Ginger– Helps increase circulation and dissolves fibrin in the blood vessels.
- Rosemary – Stimulates the circulation.
- Asparagus – Helps prevent rupturing and also strengthens the capillaries and veins. Asparagus is rich in numerous vitamins and minerals like vitamins A, C, E and K, as well as fiber, folate and chromium. It is also high in calcium, niacin, phosphorus and amino acids.
- Avocados – Rich in glutathione, which helps protect the arteries, veins and heart from oxidant damage.
- Watercress – Rich source of vitamin K, B1, B2, B6, C, E, manganese and carotenes plus iron, calcium, copper and fiber.
- Foods high in Rutin – Is a vasoprotective (protects of blood vessels), anti-inflammatory, antithrombotic, (protect against blood clots) and antioxidant. Natural sources of Rutin are apple, buckwheat, grapes, cherries, apricots and blackberries.
OTHER MEASURES4
- Horse chestnut tincture and king’s clover infusions may be useful for varicose veins.
- Losing excess weight is crucial for those who are overweight. Strain on the veins, created by carrying too much body fat, is associated with an increased risk of developing this condition.
- Regular exercise helps to burn off calories.
REFERENCES
- Dr. Das S. A manual on Clinical Surgery. 13threv.ed. Kolkata: Dr. S. Das; 2018. 648p.
- Lilienthal, S. Homoeopathic therapeutics. Philadelphia: Boericke & Tafel; 1907.
- Clarke JH.The prescriber.6thred.NewDelhi:B. Jain Publishers (P) LTD.; 2011.
- URSELL A. The Complete Guide Healing Foods. 1strev.ed. London: Dorling Kindersley Ltd., 2000. 256p.
- Boericke W. Pocket Manual of Homoeopathic Materia Medica. New Delhi: B. Jain Publishers (P) Ltd.; 2011.



