Definition
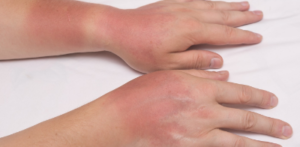 Cellulitis is usually characterised by erythema and skin warmth localised to a well-demarcated area of the leg and may be associated with an obvious source of entry of infection (e.g. leg ulcer or insect bite). The patient may be febrile and systemically unwell.1 It is a non- supportive inflammation spreading along the subcutaneous tissues and connective tissue plane and across intercellular spaces.2
Cellulitis is usually characterised by erythema and skin warmth localised to a well-demarcated area of the leg and may be associated with an obvious source of entry of infection (e.g. leg ulcer or insect bite). The patient may be febrile and systemically unwell.1 It is a non- supportive inflammation spreading along the subcutaneous tissues and connective tissue plane and across intercellular spaces.2
The term is a misnomer, as the lesion is one of the connective and interstitial tissue and not of the cells. The causative organism is mostly the Streptococcus pyogenes, though variety aerobic and anaerobic bacteria may produce cellulitis.1
Pathology
The organism usually gains access through a wound or scratch or following surgical incision. There is wide spread swelling and redness at the area of inflammation, but without definite localisation. Initially the site of inoculation becomes red. Gradually the skin swells and becomes shiny. In severe infections blebs and bullae form on the skin. Central necrosis may occur at a later stage.1, 2, and 3
Clinical Features
- In cellulitis, pain may be disproportionately intense in relation to the visible cutaneous features or may spread beyond the zone of erythema. The infection spreads quickly along the fascial plane.1
- The affected part is very much swollen and painful.
- There is varying degree of fever and toxaemia.
- Diabetic individual often suffers from cellulitis.1
On examination:
- The affected part is warm, swollen and tender.
- There is pitting oedema and brawny in duration.
- The surrounding lymph vessels may be seen as red streaks due to lymphangitis. The regional lymph nodes will be enlarged and tender with acute lymphadenitis.1, 2
- The patient usually has malaise, fever and leucocytosis, and streptococcal serology will often be positive. Legs (cellulitis) are most often affected and the site is hot, painful, erythematous andoedematous. Blistering often occurs and may be haemorrhagic.1
- Fever and a raised, indurated, tender area with indistinct margins mostly on the head and neck, particularly the buccal and preseptal areas are common. Orbital cellulitis is uncommon, and is distinguished from preorbital cellulitis based on the presence of proptosis, chemosis, impaired vision, limitation of extraocular movements, and pain with eye movement.3
Causes
- The main bacteria involved in cellulitis are Streptococcus and Staphylococcus. Cellulitis may occur anywhere on the body, but the leg is the most common site of the infection.1,3
- Cellulitis due to aureus often spreads from a central site of localized infection, such as an abscess or an infected foreign body, and is referred to as “purulent cellulitis.”2
- Wide variety of exogenous flora. In this case, a thorough history and epidemiologic data may help identify the cause. Examples of exogenous bacteria causing cellulitis include the following: Pasteurella multocida after a cat or dog bite; Capnocytophagacanimorsus after a dog bite; Eikenellacorrodens after a human bite; aeruginosa in association with ecthymagangrenosum in neutropenic pts, a penetrating injury (stepping on a nail), or hottubfolliculitis; Aeromonas hydrophila after a laceration sustained in fresh water; or Erysipelothrixrhusiopathiae after contact with domestic swine and fish.2
Diagnosis
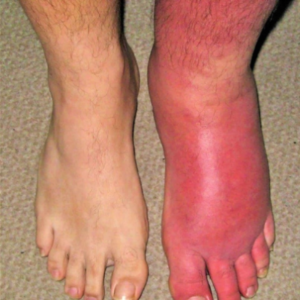 In many patients, one eschar or more develops,surrounded by an area of cellulitis and enlargement of regional lymph nodes. The incubation period is about 9 days.1
In many patients, one eschar or more develops,surrounded by an area of cellulitis and enlargement of regional lymph nodes. The incubation period is about 9 days.1
Prompt diagnosis and immediate start of treatment is required to prevent further lymphatic damage and worsening of existing elephantiasis. Relief can be obtained by removal of excess tissue but recurrences are probable unless new lymphatic drainage is established.1
If cellulitis is suspected, serum inflammatory markers, skin swabs and blood cultures should be sent, to find causative bacteria 1
If there is drainage, an open wound, or an obvious portal of entry, Gram’s staining and culture may identify the etiology. Aspiration or biopsy of the leading edge of the cellulitic tissue yields a diagnosis in only 20% of cases.2
Treatment
Topical treatment
Superficial localised skin infections like impetigo and superficial folliculitis may respond to rigorous topical treatment sometimes.
Conventional treatment is usually with intravenous antibiotics based on culture and antibiotic sensitivity. Milder cases may be treated with oral antibiotics. If cases are untreated, sequelae include lymphoedema, cavernous sinus thrombosis, sepsis and glomerulonephritis.1
Treatment includes prolonged bed rest, limb elevation, elastic stockings, meticulous skin hygiene, avoidance of local injury and prompt treatment with antibiotics if cellulitis occurs.3
Duration of treatment is 5 to 7 days for superficial infections and up to 3 weeks for deep infections.3
- Rest and elevation of the part to reduce oedema.1
- Appropriate antibiotic preferably broad spectrum should be administered.1
- Failure of inflammatory swelling to subside after 48 to 72 hours suggests that an abscess has developed. In that case incision and drainage of the pus should be accomplished.1
Homeopathy Management
There are medicines in homeopathy which can be given to heal and absorb the pus and reduce the intensity of systemic infection. But medicines should be taken in consultation with a registered homeopathic practitioner. Few medicines which are known to be very effective for cellulitis and their indications are detailed below for reference. Kindly use this information in consultation with a registered homeopathic practitioner.
Cellulitis Medicines
 APIS MELLIFICA
APIS MELLIFICA
Acts on cellular tissues causing oedema of skin and mucous membranes.The very characteristic effects of the sting of the bee furnish unerring indications for itsemployment in disease.Swelling or puffing up of various parts, oedema, red rosy hue, stinging pains, soreness,intolerance of heat, and slightest touch, and afternoon aggravation are some of the generalguiding symptoms.
 BELLADONA
BELLADONA
It has a marked action on the vascular system, skin and glands. Belladonna always is associated with hot, red skin, flushed face, glaring eyes, throbbing carotids, excited mental state, hyperaesthesia of all senses, delirium, restless sleep, dryness of mouth and throat with aversion to water, neuralgic pains that come and go suddenly.
Dry and hot; swollen, sensitive; burns scarlet, smooth.Erythema; pustules on face.Indurations after inflammations.
 CROTALUS HORRIDUS
CROTALUS HORRIDUS
Swelling and discoloration, skin tense and shows every tint of colour, with excruciating pain.Vesication.Great sensitiveness of skin of right half of body. Purpura haemorrhagica. Haemorrhage from every part of body.Dissecting wounds.Pustular eruptions.Insect stings.Lymphangitis and septicaemia. Boils, carbuncles, and eruptions are surrounded by purplish, mottled skin and oedema.
PYROGENIUM
Great pain and violent burning in abscesses.Chronic complaints that date back to septic conditions.Threatening heart failure in zymotic and septic fevers.Small cut or injury becomes much swollen and inflamed-discolored.Pyrogen is the great remedy for septic states, with intense restlessness.“In septic fevers, especially puerperal, Pyrogen has demonstrated its great value as ahomoeopathic dynamic antiseptic.
 SILICEA
SILICEA
It is related to all fistulous burrowings.Ripens abscesses since it promotes suppuration.Felons, abscesses, boils, old fistulous ulcers.Scars suddenly become painful.Pus offensive.Promotes expulsion of foreign bodies from tissues.
Every little injury suppurates.Long lasting suppuration and fistulous tracts.
References
- Ralston S.H., Penman I.D., Strachan M.W.J., Hobson R.P. Davidson’s, Principles and Practice of Medicine. 17thed. Edinburgh; New York: Churchill Livingstone; 1995. 1203p.
- Kasper D.L., Fauci A.S., Hauser S.L., Longo D.L., Jameson J.L., Loscalzo J. Harrison’s Manual of Medicine. 19th ed.United States: McGraw Hill; 2016. 1222p.
- API Textbook of Medicine. 9thed. Mumbai: The Association of Physicians of India, Jaypee Brothers Medical Publishers (P) Ltd; 2012. 2066p
- Boericke W. New Manual of Homœopathic Materia Medica and Repertory. 9th Reprinted Edition. New Delhi: B Jain Publishers (P) Ltd; 2005.
- Lilienthal, S. Homoeopathic therapeutics. Philadelphia: Boericke& Tafel; 1907
