 The usual victims of Buerger’s disease are young men below 40 years of age. It is the inflammatory reaction in the arterial wall with involvementof the neighboring vein and nerve, terminating in thrombosis of the artery.1, 2, 4
The usual victims of Buerger’s disease are young men below 40 years of age. It is the inflammatory reaction in the arterial wall with involvementof the neighboring vein and nerve, terminating in thrombosis of the artery.1, 2, 4
The lesions are segmental and usually begin in arteries of small and medium size.1, 3, 4
Bothupper and lower extremities are affected. In lower extremity the disease generally occurs beyondpopliteal artery, starting in tibial arteries extending to the vessels of the foot. The disease hasalso affected the arteries of the G.T. tract, lungs and heart. Early in the course of Buerger’s disease the superficial veins are involved producing the characteristic migratory, recurrent superficialphlebitis.1
Aetiology
This disease has a striking association with cigarettesmoking. Majority patients of Buerger’s disease come from lower socio-economic groups. An autoimmune etiology has been postulated and familial predisposition has been reported.The pedal/feet arteries are involved first and the patients complain of pain while walking at thearch of the foot (foot claudication), somewhat less often at the calf of the leg, but never at thethigh or buttock (which is common in atherosclerosis).1, 2
It often remits if the patient stops smoking.2
Symptom
- Pain is typical of intermittent claudication,which progresses to ‘rest pain’.
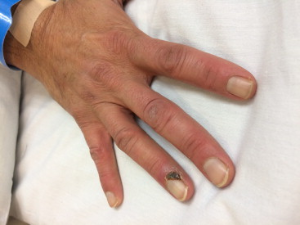
- Gradually postural color changes appear followed by trophicchanges and eventually ulceration and gangrene of one or more digits and finally of the entirefoot or hand may ensue.
 Signs
Signs
- Buerger’s test will be positive.1
- Buerger’s disease can be differentiatedfrom Raynaud’s disease by sex incidence, the extremity affected and disappearance of peripheralpulses. It is differentiated from senile gangrene by the age, by its association with superficialphlebitis and pitting oedema.1
- Characteristic arteriographic appearance of this disease is the smoothand normal appearance of larger arteries combined with extensive occlusion of the smaller arteriesalong with extensive collateral circulation.1
- Wrist and ankle pulses are absent but brachial and popliteal pulses are present.2
Complication
lschaemic or Arterial ulcer.-These ulcers are rare compared to venous ulcer. Arterial ulcers are due to peripheral arterial disease (atherosclerosis is the commonest followed by Buerger’s disease) and poor peripheral circulation. This condition is more often seen in older people and in episodes of trauma and infection of the destroyed skin over a limited area of the leg or the foot.1
When it occurs secondary to Buerger’s disease, younger men between 20 and 40 years of age are affected. In this case patches of dry gangrene may be present along with arterial ulcer. Such ulcers tend to occur on the anterior and outer aspects of the leg, dorsum of the foot, on the toes or the heel (the parts exposed to trauma). Unlike venous ulcer (which is painless) pain is the main complaint of this disease. When this ulcer occurs on the inner side of the ankle, possibility of venous ulcer should be excluded. Venous ulcer usually occurs above the medial malleolus, whereas arterial ulcer tends to occur below the medial malleolus. Moreover there is often a history of intermittent claudication and even rest pain in majority of cases of arterial ulcer. If the leg is kept elevated above the heart level, the ulcer shows no sign of healing and the patient will complain of pain in this position.1
Major limb amputation is the most frequent outcome if patients continue to smoke.2
Treatment
If the ulcer seems to be due to Buerger’s disease (ischaemic), the wholebody must be examined for presence of atherosclerosis or its complication anywhere in thebody. Moreover Buerger’s disease is a bilateral condition and the other limb should always beexamined.1
These ulcers are punched out with destruction of the deep fascia (cf. venous ulcer). The tendons, bone or underlying joints may be exposed in the floor of the ulcer which is covered by minimal granulation tissue. Peripheral arterial pulses should always be felt. Pulse of dorsalis pedis artery is almost always either feeble or absent. Presence of ischaemic changes can be detected in the foot e.g. pallor, dry skin, loss of hair, fissuring of nails etc. Arteriography is important to detect the arterial disease.1
Symptomatic therapy with vasodilators such as prostacyclin and calcium antagonists or sympathectomy is the conventional therapy approach. 2
Treatment is primarily cessation of smoking. This helpshalt the progression of the disease but does not lead to reversalof the established occlusion. Sympathectomy for pain relief isalso done. Stem cell therapy has also been tried.3
Imaging with CT, MR, or conventional angiography shows smooth tapering lesions in distal vessels, often without proximal atherosclerotic disease. Abstinence from tobacco is essential.4
Scope of Homeopathy
Homeopathy is given for reducing the inflammation. Cessation of smoking is a must whatever therapy is used.
Some medicines which are found useful for such pathology are detailed below but must be taken in consultation with a skilled homeopathic practitioner.
Medicines5
 1. Anthracinum
1. Anthracinum
Gangrene, foul secretions, hemorrhages, black, thick, tar like, rapidly decomposing.
 2. Arnica Montana
2. Arnica Montana
Skin black and blue, itching burning eruption. Deathly coldness of forearm. Thrombosis. Ulcers, chronic spreading. Gangrene.
 3. Arsenic Album
3. Arsenic Album
Burning, restlessness and tingling of extremities.
 4. Carbo Animalis
4. Carbo Animalis
Malignant ulcers, Blue venous plethora. Cicatrices become painful. Copper colored eruptions. Red spots. Smooth indurated.
 5. Crotalus Horridus
5. Crotalus Horridus
Hands feel numb, start trembling or become swollen. Boils carbuncles, surrounded by bluish skin.
 6. Lachesis Muta
6. Lachesis Muta
Toes feel broken, feet feel sweaty or have trembling or prickling of hands. Gangrene, dissecting wounds.
 7. Plumbum Metallicum
7. Plumbum Metallicum
Hands and feet cold. Stinging and tearing in limbs also twitching and tingling, numbness, pain or tremor.
 8. Secale Cornutum
8. Secale Cornutum
Cold, dry hands and feet of excessive smokers with feeling of fuzziness in fingers. Trembling staggering gait. Fingers and feet bluish, numb, violent cramps. Icy coldness of extremities, tingling of toes, dry gangrene, formication under skin.
References
- Dr. Das S. A manual on Clinical Surgery. 13threv.ed. Kolkata: Dr. S. Das; 2018. 648p.
- Ralston S.H., Penman I.D., Strachan M.W.J., Hobson R.P. Davidson’s, Principles and Practice of Medicine. 23rd rev.ed. Edinburgh; Churchill Livingstone/Elsevier; 2018. 1417p.
- API Textbook of Medicine. 9th rev.ed. Mumbai: The Association of Physicians of India, Jaypee Brothers Medical Publishers (P) Ltd; 2012. 2066p.
- Kasper D.L., Fauci A.S., Hauser S.L., Longo D.L., Jameson J.L., Loscalzo J. Harrison’s Manual of Medicine. 19th rev. Ed.United States: McGraw Hill; 2016. 1222p.
