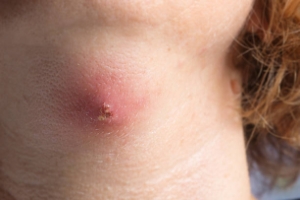
 ABSCESS. - An abscess is a collection of pus within the body. Abscess can be of classified into various types based on its character:
ABSCESS. - An abscess is a collection of pus within the body. Abscess can be of classified into various types based on its character:
(i) Pyogenic Abscess. - This is the commonest variety of abscess and may result from cellulites or acute lymphadenitis. The organisms gain entry either directly through the penetrating wound or local extension from adjacent focus of infection or haematogenous or lymphatic spread from a distance. At first the infected part becomes red hot and quite tender. When pus develops, the pain takes a typical character of throbbing in nature. There will be brawny induration and oedema (demonstrable by pitting on pressure). Fluctuation may or may not be present (as in parotid abscess).2
(ii) Pyaemic Abscess. - These are generally multiple in numbers, either develops simultaneously or a number of them crop up in succession only after one has been incised. This condition results when infective emboli circulating in the blood lodge in different parts of the body and give rise to multiple abscesses. The peculiarities of these abscesses are that they commonly occur in the subfascial plane and do not present the features of a common abscess. These are non-reacting in nature i.e. acute features are absent. But constitutional disturbances are tremendous with high fever, rigor and toxaemia.2
(iii) Cold Abscess. - As the name suggests, this abscess is cold and non-reacting in nature. It does not produce hot and painful abscess as seen in pyogenic abscess. Brawny induration, oedema and tenderness are conspicuous by their absence. Cold abscess is almost always a sequel of tubercular infection anywhere in the body commonly in the lymph nodes and bone. Caseation of the lymph nodes forms the cold abscess. The commonest sites are at the neck and axilla. Sometimes cold abscesses are seen at the loin, at the back or at the side of the chest wall. These are sequel of tuberculosis affection of the spine, ribs and posterior mediastinal group of lymph nodes? Cold Abscesses may also originate from the ends of the bones and joints and gradually come to the surface through the fascial planes.2
ANORECTAL ABSCESSES
Perianal abscesses develop between the internal and externalanal sphincters and may point at the perianal skin. Ischiorectalabscesses occur lateral to the sphincters in the ischiorectal fossa.They usually result from infection of anal glands by normal intestinalbacteria. Crohn’s disease is sometimes responsible.Patients complain of extreme perianal pain, fever and/or discharge of pus. Spontaneous rupture may lead to thedevelopment of fistulae. These may be superficial or track throughthe anal sphincters to reach the rectum. Abscesses are drainedsurgically and superficial fistulae are laid open with care to avoidsphincter damage.1
CEREBRAL ABSCESS
Bacteria may enter the cerebral substance through penetratinginjury, by direct spread from paranasal sinuses or the middle ear, or secondary to sepsis. Untreated congenital heart disease is arecognized risk factor. The site of abscess formation and the likelycausative organism are both related to the source of infection. Initial infection leads to local suppuration followedby loculation of pus within a surrounding wall of gliosis, which in a chronic abscess may form a tough capsule. Haematogenous spread may lead to multiple abscesses.1
A cerebral abscess may present acutely with fever, headache, meningism and drowsiness, but more commonly presents overdays or weeks as a cerebral mass lesion with little or no evidenceof infection. Seizures raised intracranial pressure and focalhemisphere signs occur alone or in combination. Lumbar puncture is potentially hazardous in the presence ofraised intracranial pressure and CT should always precede it. CT reveals single or multiple low-density areas, which show ringenhancement with contrast and surrounding cerebral oedema. There may be an elevated white blood cell countand ESR in patients with active local infection. The possibilityof cerebral toxoplasmosis or tuberculosis disease secondary to IV infection should always be considered.1Antimicrobial therapy is indicated once the diagnosis is made. The likely source of infection should guide the choice of antibiotics. Some cases come under scope of neurosurgery and need that intervention.
INTRAABDOMINAL ABSCESSES
Generally diagnosed through radiographic studies, ofwhich abdominal CT is typically most useful.3
INTRAPERITONEAL ABSCESSES
- Epidemiology: Of intraabdominal abscesses, 74% are IP or retroperitoneal, notvisceral.3
- Pathogenesis: Most IP abscesses arise from colonic sources. Abscesses develop in untreated peritonitis as an extension of the disease process and represent hostdefense activity aimed at containing the infection.3
- Microbiology: Infection is typically polymicrobial; the most frequently isolatedanaerobe is Bacteroides fragilis.3
Treatment
- Antimicrobial therapy is adjunctive to drainage and/or surgical correction of anunderlying lesion or process.
– Diverticular abscesses usually wall off locally, and surgical intervention is notroutinely needed.
– Antimicrobial agents with activity against gram-negative bacilli and anaerobic organisms are indicated.3
VISCERAL ABSCESSES
- Liver Abscess
- Epidemiology, Pathogenesis, and Microbiology:Liver abscesses account for up to half of visceral intraabdominal abscesses and are caused most commonly by biliary tractdisease (due to aerobic gram-negative bacilli or enterococci) and less often by localspread from pelvic and other IP sources (due to mixed flora including aerobic andanaerobic species, among which B. fragilis is most common) or hematogenous seeding (infection with a single species, usually S. aureus or streptococci such as S. milleri).3
– Amebic liver abscesses are not uncommon, with positive serology in >95% ofaffected patients.3
- Clinical manifestations: Patients have fever, anorexia, weight loss, nausea, and vomiting, but only ~50% have signs localized to the RUQ, such as tenderness, hepatomegaly,and jaundice. Serum levels of alkaline phosphates are elevated in ~70% of pts, andleukocytosis is common. One-third to one-half of patientsis bacteremic.3
Treatment
- Drainage is the mainstay of treatment, but medical management with longcourses of antibiotics can be successful.3
– Empirical therapy is the same as for intraabdominal sepsis and secondarybacterial peritonitis.
Percutaneous drainage tends to fail in cases with multiple, sizable abscesses; with viscous abscess contents that plug the pigtail catheter; with associateddisease (e.g., of the biliary tract) requiring surgery; with the presence of yeast;or with lack of response in 4–7 days.3
- Splenic Abscess
- Epidemiology and Pathogenesis: Splenic abscesses are much less common than liverabscesses and usually develop via hematogenous spread of infection (e.g., due toendocarditis). The diagnosis is often made only after the patient’s death; the condition isfrequently fatal if left untreated.3
- Microbiology: Splenic abscesses are most often caused by streptococci; S. aureus is the next most common cause. Gram-negative bacilli can cause splenic abscess in ptswith urinary tract foci, with associated bacteremia, or with infection from another intranabdominal source; salmonellae are fairly commonly isolated, particularly frompts with sickle cell disease.3
- Clinical manifestations: Abdominal pain or splenomegaly occurs in ~50% of casesand pain localized to the LUQ in ~25%. Fever and leukocytosis are common.3
Treatment
Patients with multiple or complex multilocular abscesses should undergo splenectomy, receive adjunctive antibiotics, and be vaccinated against encapsulated organisms (Streptococcus pneumonia, Haemophilus influenza, and Neisseriameningitidis). Percutaneous drainage has been successful for single, small (<3-cm) abscesses and may also be useful for pts at high surgical risk.3
- Perinephric and Renal Abscesses
- Epidemiology and Pathogenesis: Perinephric and renal abscesses are uncommon.More than 75% of these abscesses are due to ascending infection and are preceded by pyelonephritis. The most important risk factor is the presence of renal calculithat produce local obstruction to urinary flow.3
- Microbiology: E. coli, Proteus spp. (associated with struvite stones), and Klebsiellaspp. Are the most common etiologic agents; Candida spp. is sometimes identified.3
- Clinical manifestations: Clinical signs are nonspecific and include flank pain, abdominal pain, and fever. This diagnosis should be considered if pts with pyelonephritishave persistent fever after 4 or 5 days of treatment, if a urine culture yields a polymicrobial flora, if the pt has known renal stone disease or if fever and pyuriaoccur in conjunction with a sterile urine culture.3
Treatment
Drainage and the administration of antibiotics active against the organismsrecovered are essential. Percutaneous drainage is usually successful for perinephric abscesses.3
SCOPE OF HOMEOPATHY
Abscess falls within the scope of homeopathy. The remedy is being chosen based on pathology, location, peculiar characteristic symptoms found on examination, type of pain etc. Self prescription is not advisable and homeopathic treatment shall be started in consultation with a registered and skilled homeopathic practitioner.
MEDICINES FOR ABSCESS with their symptoms4, 5
 Apis Mellifica
Apis Mellifica
Diffuse inflammation of the cellular tissues, ending in their destruction: stinging, burning pains in incipient abscesses.
 Arnica Montana
Arnica Montana
Hot, hard shining swelling; pricking pains and dull stitches in the part; general sinking of strength.
 Arsenicum Album
Arsenicum Album
Intolerable burning pains during the fever or when the abscess threatens to become gangrenous; pus copious, bloody, corroding, ichorous, watery, and of a putrid smell; great debility, muscular prostration, sleeplessness and restlessness.
 Baryta Carb
Baryta Carb
Inflammation of the cellular tissue, passing over into suppuration; incipient suppuration of glands; boils and furuncles.
 Belladonna
Belladonna
Pressure, burning and stinging in abscess; scarlet redness and hot swelling; pus scanty, cheesy and flocculent; great sensitiveness to cold air. Hepatic abscess or other glandular abscesses.
 Calcarea Sulphurica5
Calcarea Sulphurica5
In cases of abscess where the suppuration is prolonged. The presence of pus with a vent is an indication. It comes in after Silicea.
 Calendula Officinalis
Calendula Officinalis
Induration after surgical operations, followed by suppuration; the wound looks raw and inflamed, with stinging pains, followed by throbbing, as if it would suppurate; profuse and exhausting suppuration in traumatic abscess.
 Hepar Sulphur
Hepar Sulphur
Lacerating and pricking pains in the tumors; throbbing and beating in the abscess, the skin over the abscess is highly inflamed, hard, hot and swelling; pus scanty, bloody, corroding smelling like old cheese; pains worse at night and by exposure to cold.
 Lachesis Muta 5
Lachesis Muta 5
In low conditions of abscess when the pus is thin, dark, and offensive in character. The inflamed parts are purplish in color. Abscesses from poisonous matter introduced into the system.
 Mercurius Solubilis
Mercurius Solubilis
SLOWLY SUPPURATING ABSCESSES. Burning redness of the skin, with prickling and tingling sensation; hard, hot, inflammatory swelling, pressing from within outward; pulsating pains; pus copious, bloody, corroding, thin and watery; or all these characters, but scanty.
 Rhus Toxicodendron
Rhus Toxicodendron
ABSCESSES OF AXILLARY OR PAROTID GLANDS, swelling painful to touch, and discharging bloody-serous pus, with stinging and gnawing pains. Smooth, red and shining swellings, the inflamed skin being covered with little painful white vesicles.
 Silicea Terra
Silicea Terra
It controls the suppurative process; seeming to mature processes when desired, and certainly reducing excessive suppuration to moderate limits. Pains of abscess are either burning, cutting, itching, prickling or pulsative. Pus copious or scanty, bloody brownish, corroding, gelatinous, gray or greenish, putrid, thin and watery, or yellow. After matter has been discharged, it promotes granulation and cicatrization.
 Sulphur
Sulphur
CHRONIC ABSCESS, tendency to suppuration, dependent upon a psoric or scrofulous diathesis; pains throbbing or stinging, and after evacuation of the pus there is a tendency to ulceration.
IN SCROFULOUS ABSCESSES - Calcarea carb and if about the glands of the neck Calcarea iod.
DIET RECOMMENDATION FOR ABSCESS
Foods to be taken
- Fruits and vegetables (pine apple, juices)
- Garlic
Foods to be avoided
- Fried foods
- Sugar
- White rice
- White flour
Yoga and Exercise
- General aerobic exercises like walking can be done.
- Pranayama
HOME REMEDIES
To be taken in consultation with your treating physician/ homeopath.
- Apply warm compresses to the area for about 30 minutes 4 times daily.
- Do not attempt to drain the abscess by pressing on it.
- Wash your hands thoroughly.
- Launder clothing, towels or compresses that have touched the infected area.
REFERENCES
- Ralston S.H., Penman I.D., Strachan M.W.J., Hobson R.P. Davidson’s, Principles and Practice of Medicine. 23rded. Edinburgh; Churchill Livingstone/Elsevier; 2018. 1417p.
- Dr. Das S. A manual on Clinical Surgery. 13threv.ed. Kolkata: Dr. S. Das; 2018. 648p
- Kasper D.L., Fauci A.S., Hauser S.L., Longo D.L., Jameson J.L., Loscalzo J. Harrison’s Manual of Medicine. 19th rev. ed. United States: McGraw Hill; 2016. 1222p.
- Boericke W. Pocket Manual of Homoeopathic Materia Medica. New Delhi: B. Jain Publishers (P) Ltd.; 2011
- Dewey WA.Practical homeopathic therapeutics.3rd ed.New Delhi: B. Jain Publishers (P) LTD.;2009.
